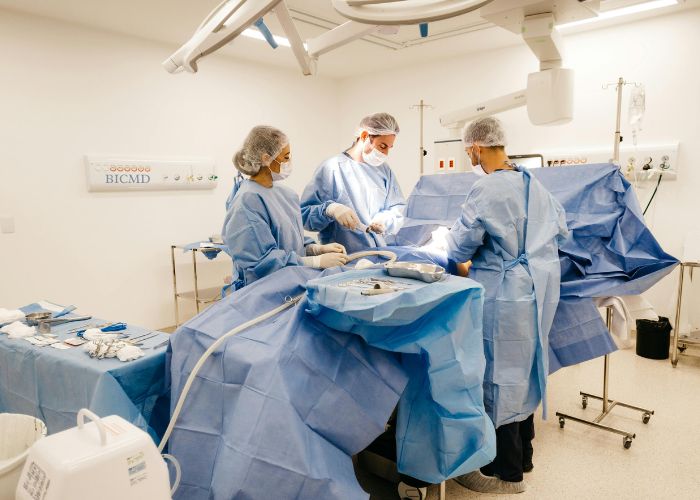
The True Cost of Surgery in Workers’ Comp: It’s Not the Surgery
Need to Know
- The biggest cost drivers in workers’ comp surgery claims aren’t the procedure; they’re what happens after
- Delays, complications, and extended care determine total claim cost
- The most important decisions are made before surgery is approved
What We See Across Workers’ Comp Surgery Claims
In workers’ compensation, most conversations still start here:
“How much does the surgery cost?”
However, across claims, that question rarely predicts the true outcome.
The better question is:
“What will this surgery cost the claim over the full recovery timeline?”
Because surgery is just one point in the process. What determines whether a claim resolves or drags on, is everything that happens during recovery.
A Common Workers’ Comp Orthopedic Scenario:
An injured worker is recommended for a rotator cuff repair after ongoing shoulder pain.
The surgery is approved quickly. The procedure itself goes as planned.
However, recovery doesn’t follow the expected path.
Range of motion improves slowly. Pain lingers longer than anticipated. Physical therapy extends well beyond the original plan. Work restrictions remain in place. Additional imaging is ordered. A second opinion is requested.
What started as a routine orthopedic case becomes a prolonged claim, not because the surgery failed, but because the recovery path wasn’t clearly defined upfront.
How Workers’ Comp Surgery Costs Actually Compound
When you step back, most claims follow a familiar pattern:
Surgery is approved → recovery delays → extended therapy → persistent symptoms → additional treatment → prolonged claim
Each step adds cost and complexity. And by the time it’s obvious, the claim is already off track.
The Gap in Early Decision-Making for Surgery Claims
What’s missing isn’t effort, it’s visibility.
Early decisions tend to focus on:
- Whether surgery is reasonable
- What the procedure will cost
But there is not enough focus on:
- Whether surgery is actually necessary
- Whether it’s the right procedure for that specific case
- What the expected recovery timeline looks like
- What risks could extend the claim
That gap is where uncertainty, and cost, gets introduced.
Why Recovery Drives Workers’ Comp Claim Cost
Across claims, the biggest cost drivers are consistent:
- Recovery timelines extend beyond expectations
- Complications introduce new procedures or setbacks
- Therapy continues without clear benchmarks
- Cases shift into long-term pain management
These aren’t outliers. They’re predictable patterns when recovery isn’t part of the upfront decision-making process.
Where Workers’ Comp Surgery Claims Break Down
Most claims don’t become expensive because of poor care.
They become expensive because decisions are made with incomplete visibility.
When there is limited:
- Validation of surgical necessity
- Alignment between procedure and expected outcome
- Planning for complications or delays
The process becomes reactive and costs follow.
What Changes When You Focus on Total Claim Cost
When decisions are made with the full lifecycle of the claim in mind, the trajectory shifts:
- Recovery becomes more predictable
- Complications decrease
- Therapy stays within expected ranges
- Return-to-work timelines improve
Instead of reacting to problems, the claim moves with a clear path forward.
Common Question: Why Do Workers’ Comp Surgery Claims Get So Expensive?
The answer is because the cost isn’t driven by the surgery itself.
Cost is driven by everything that happens after, especially when that path wasn’t clearly evaluated before the procedure.
The true cost of surgery in workers’ comp is determined before the procedure and during recovery, not just in the operating room.
Our role is to bring clarity to that process, helping align surgical decisions with realistic recovery expectations so claims resolve more efficiently and outcomes improve.
Improve Workers’ Comp Surgery Outcomes with Early Clinical Clarity
If you want to reduce delays, control costs, and keep claims moving forward, the key is making informed decisions before surgery ever happens. At BICMD, we help claims teams evaluate surgical necessity, define realistic recovery expectations, and identify risks early, so cases don’t drift into prolonged, expensive timelines. By focusing on the full lifecycle of a claim, not just the procedure, organizations can achieve faster return-to-work outcomes, fewer complications, and more predictable results. Connect with BICMD today to bring clarity and confidence to your workers’ comp surgical claims.